NYC's Hospital System Never Reached Full Capacity in Spring 2020
Plus other observations about citywide hospital data.
We know New York City hospitals experienced a dramatic drop in visits to emergency departments in spring 2020. What about inpatient census? Was the system ever out of beds or bursting at the seams?1 How many patients were placed on ventilators? Did most have covid?
In this post, I’ll speak to these and other questions using data from the New York Department of Health.2 The source file has a start date of March 26, 2020, which limits our view of city hospitals in the earliest days of the covid response and robs analysts of a proper baseline. Nevertheless, there are plenty of interesting things to see.
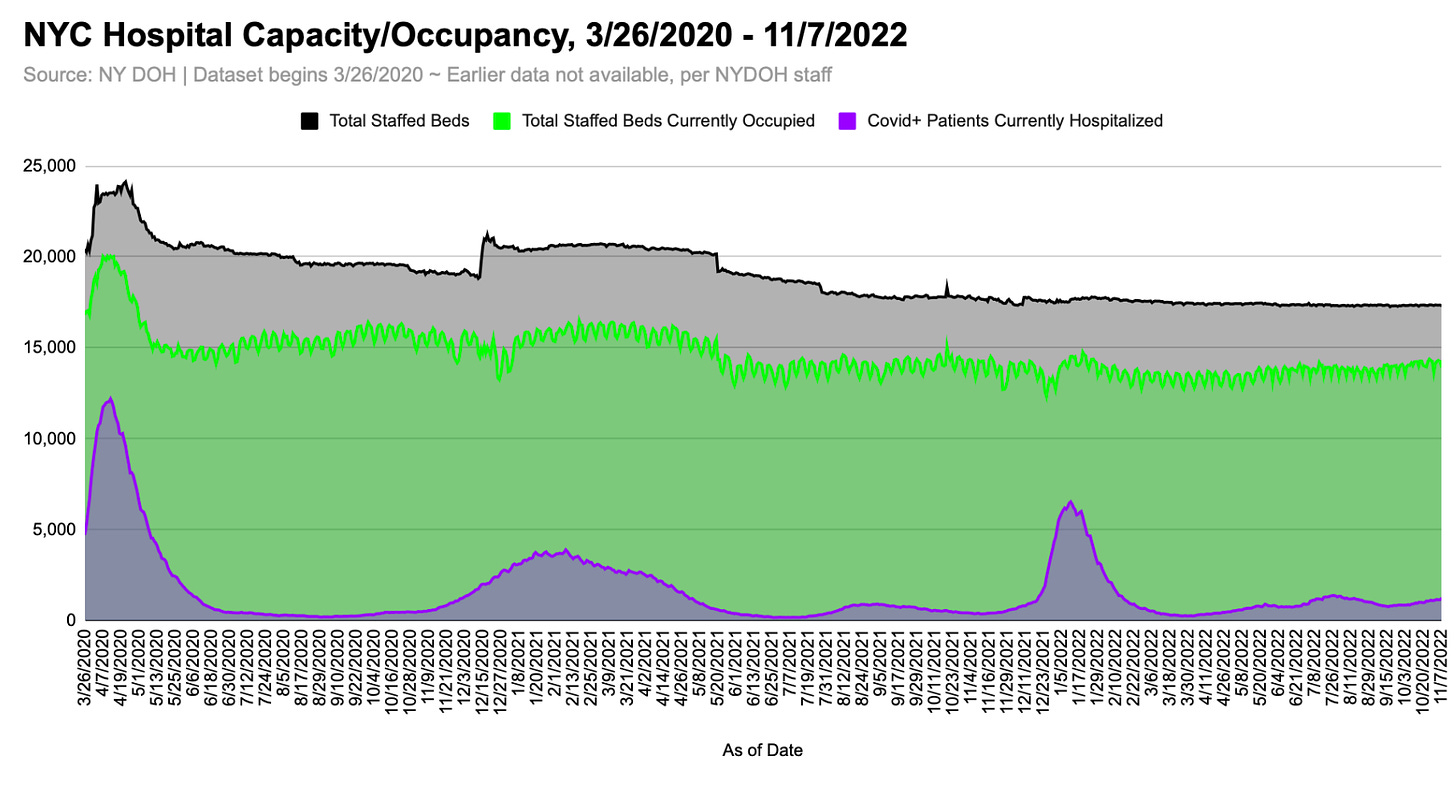
Hospital Capacity
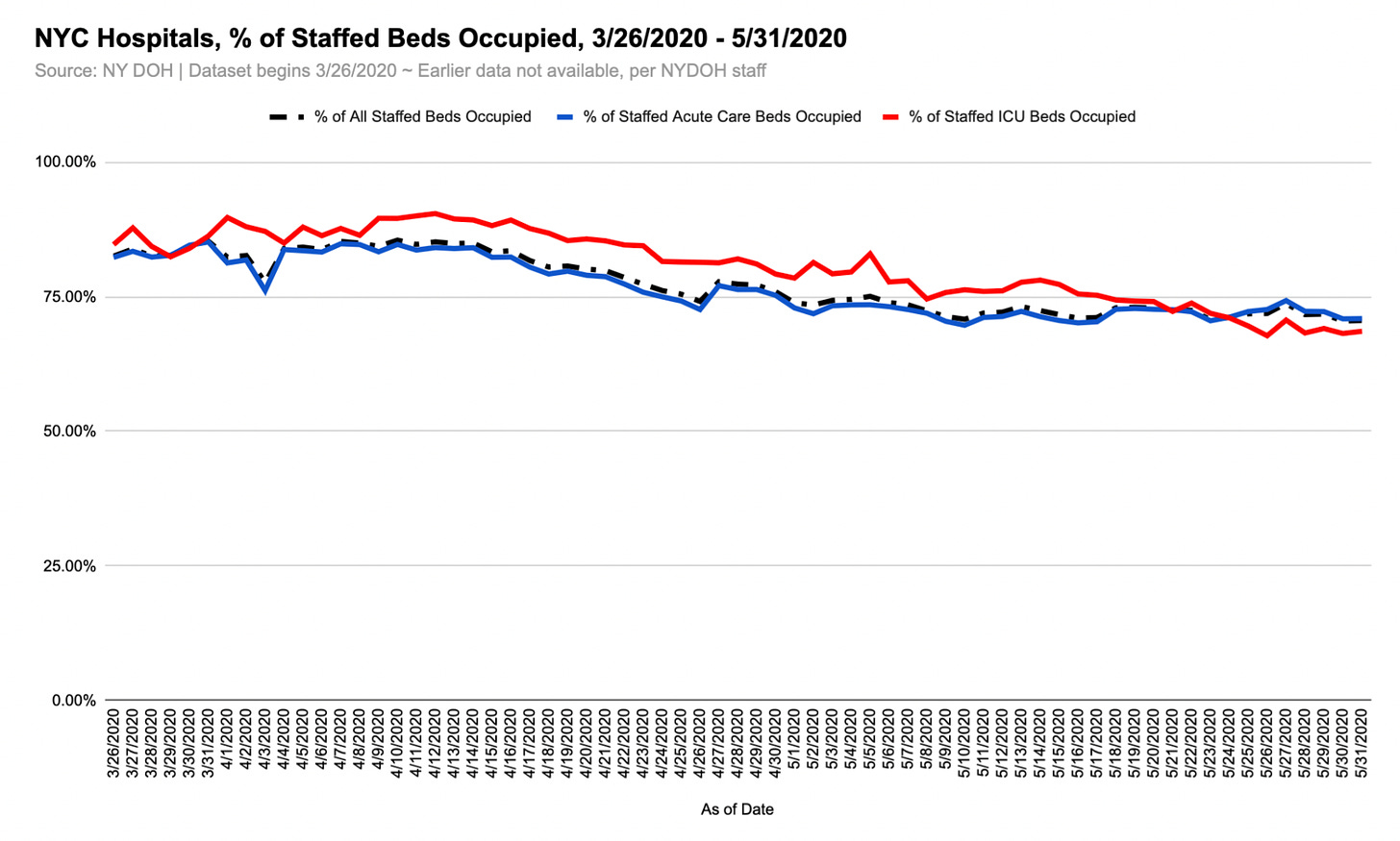
Systemwide, New York City hospitals did not reach full capacity in spring 2020. The city’s staffed acute care and ICU beds were 85% and 90% occupied, respectively, at their late March/early April peaks.
After reports that some facilities, like Elmhurst Hospital in Queens, were being inundated with visits and patients, while others had plenty of space, the state launched a “Surge & Flex” system that facilitated transfers or diversions to hospitals with higher numbers of available beds. In his book American Crisis, former New York governor Andrew Cuomo says the approach “saved lives,” resulted in nearly 1,500 patient transfers, and “help[ed] New York [state] avoid the tragic collapse of the healthcare system that we witnessed in Italy" (p. 296).
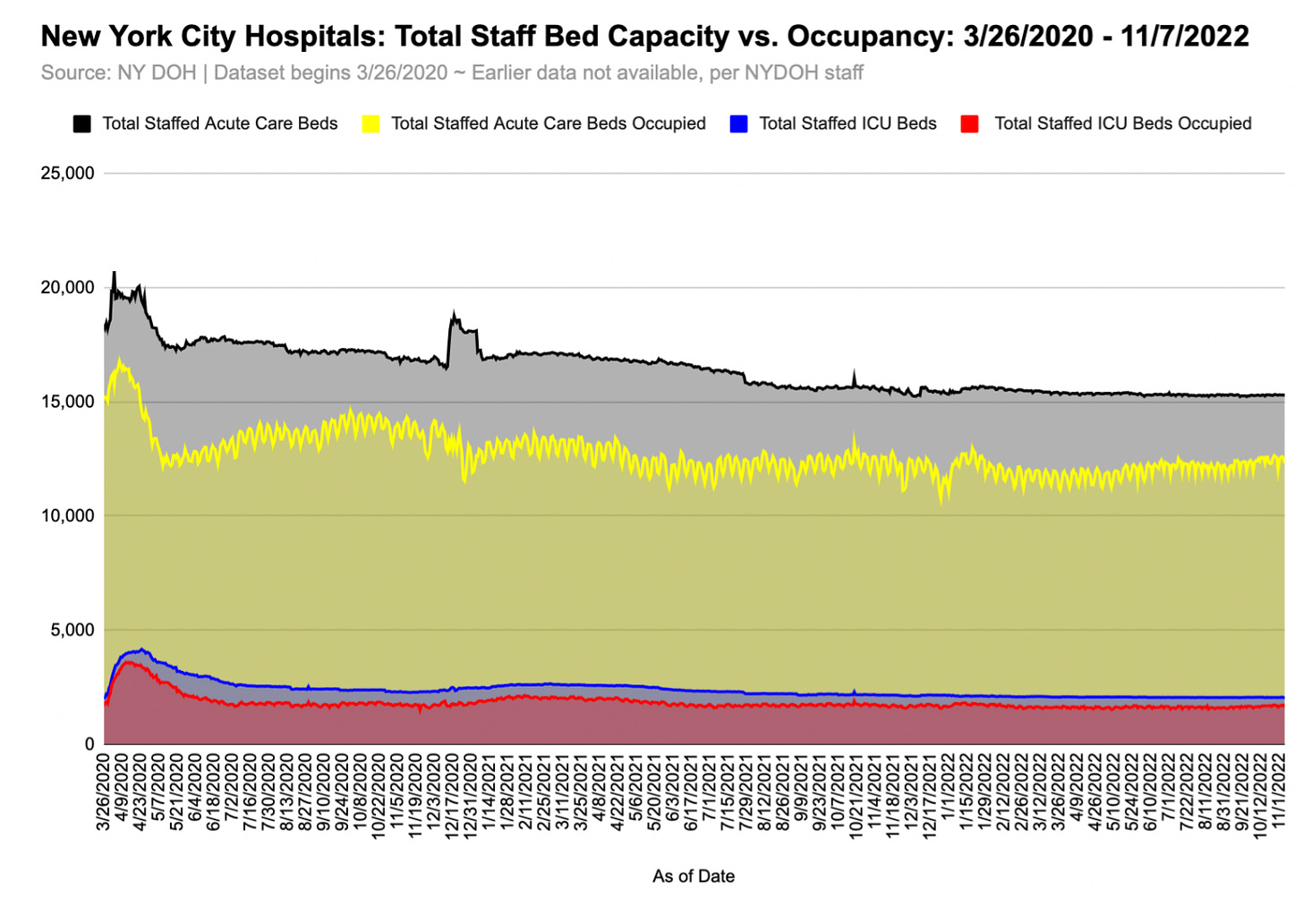
Because the number of staffed beds in NYC hospitals increased by ~3,500 between March 26th and April 17th - and occupants rose in turn - it’s tempting to conclude that the city’s hospital system would have been incapacitated if more beds had not been added.3 To substantiate such a claim, we would need more information about the patients who were being admitted.
For example, although the number of patients sent (or sent back) to nursing homes from hospitals has been the subject of much media coverage and two audits, we have no idea how many residents were admitted from those facilities to the hospitals - or why.4
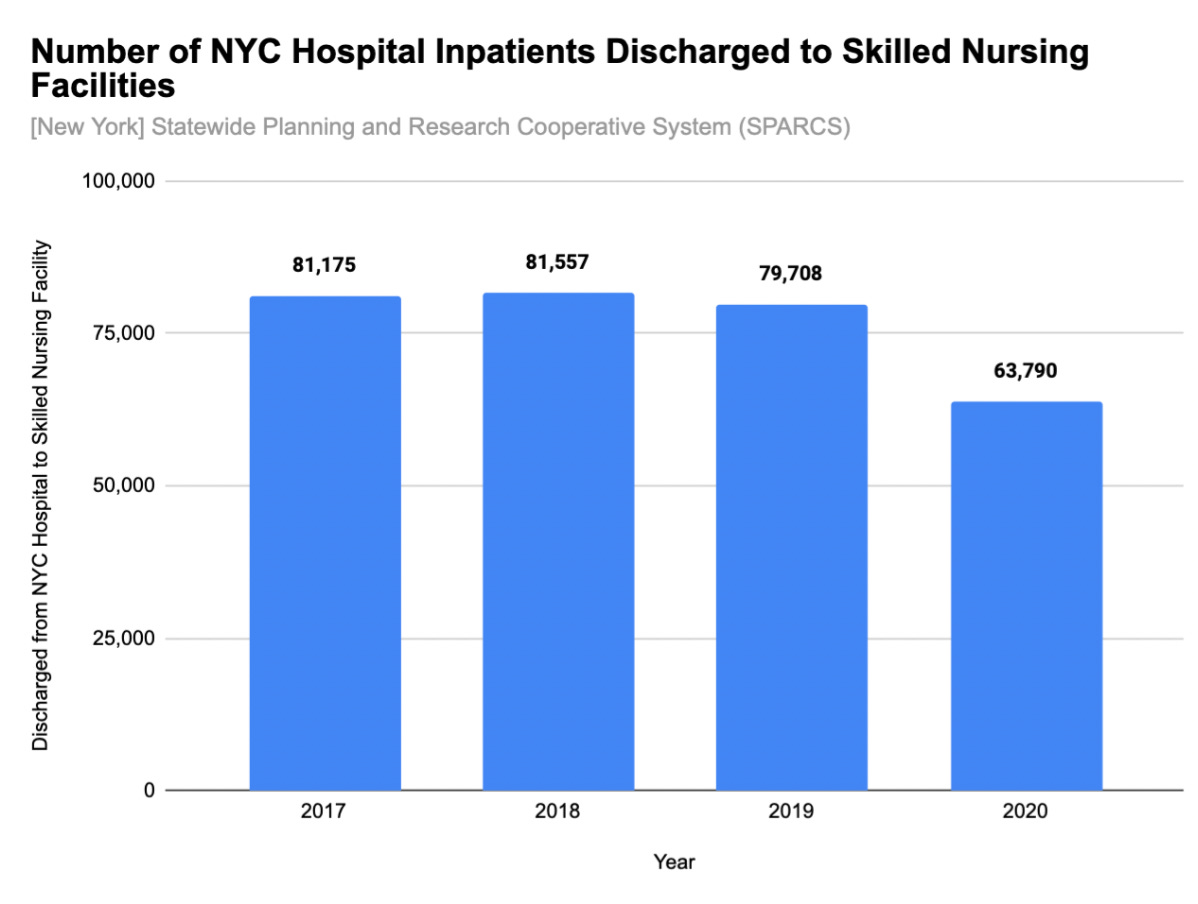
SPARCS data show a 25% decrease (n=15,918) in the number of NYC hospital inpatients discharged to skilled nursing facilities in 2020, as compared to 2019.
Resident deaths both inside and outside care of facilities likely help explain the decline. However, without discharge data by week or month, it’s impossible to determine the extent to which NYC hospitals were being used in spring 2020 to manage a fragile population that was already in managed healthcare.
It's possible that protocols, public/political pressure, and some degree of panic - versus a need arising from illness due to the sudden spread SARS-CoV-2 - fueled the push for more beds and also resulted in a higher propensity to admit patients (or certain patients, like nursing home residents) in spring 2020. Regardless, NYC’s hospital system did not come close to being over capacity.
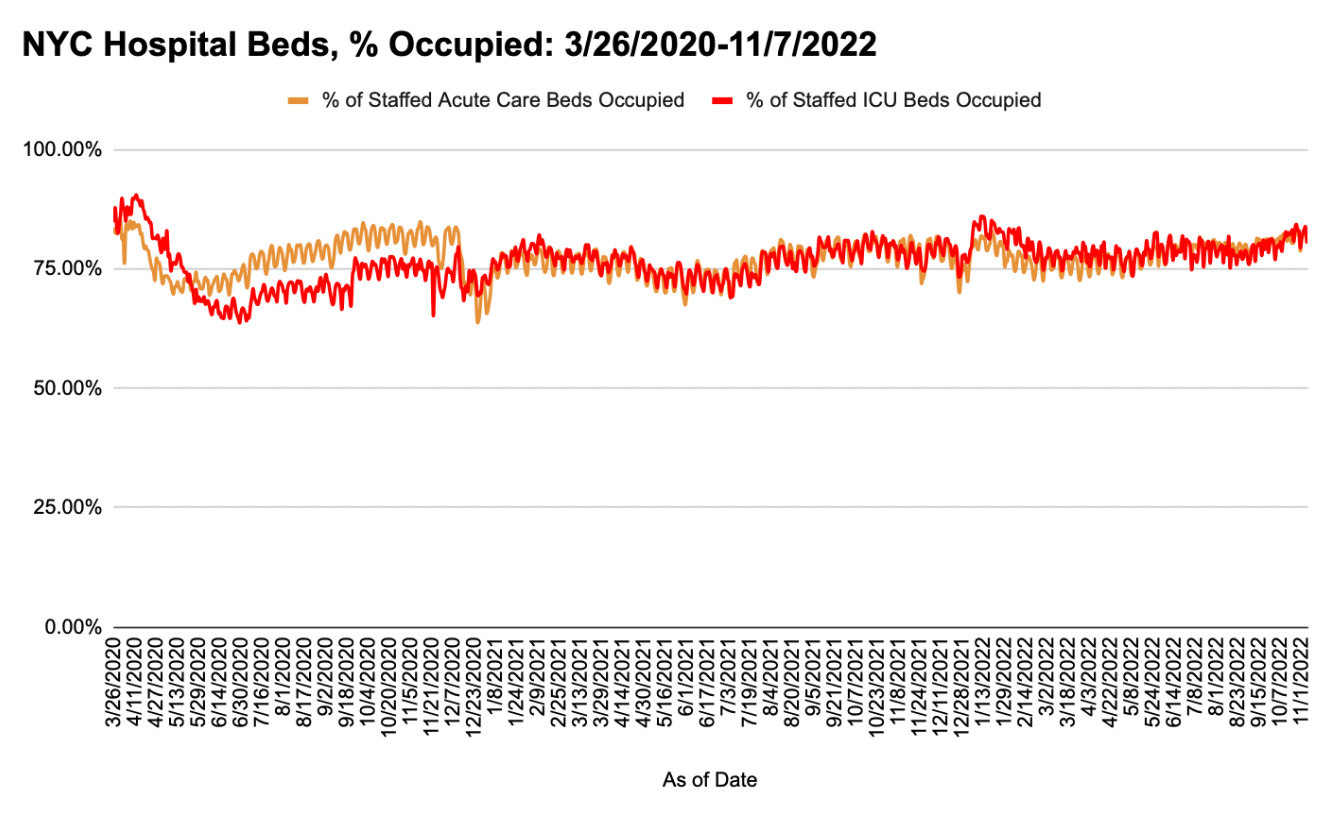
Likewise, despite recurring media reports about impending doom, patient census has continued to be non-threatening. For a better sense of how the pandemic-response (including irrational quarantine protocols, school closures, and vaccine mandates) has impacted the number of staffed beds since March 2020, we would need to see total beds and occupancy data back from January 1, 2020 onward, at least (ideally, from January 1, 2016).5
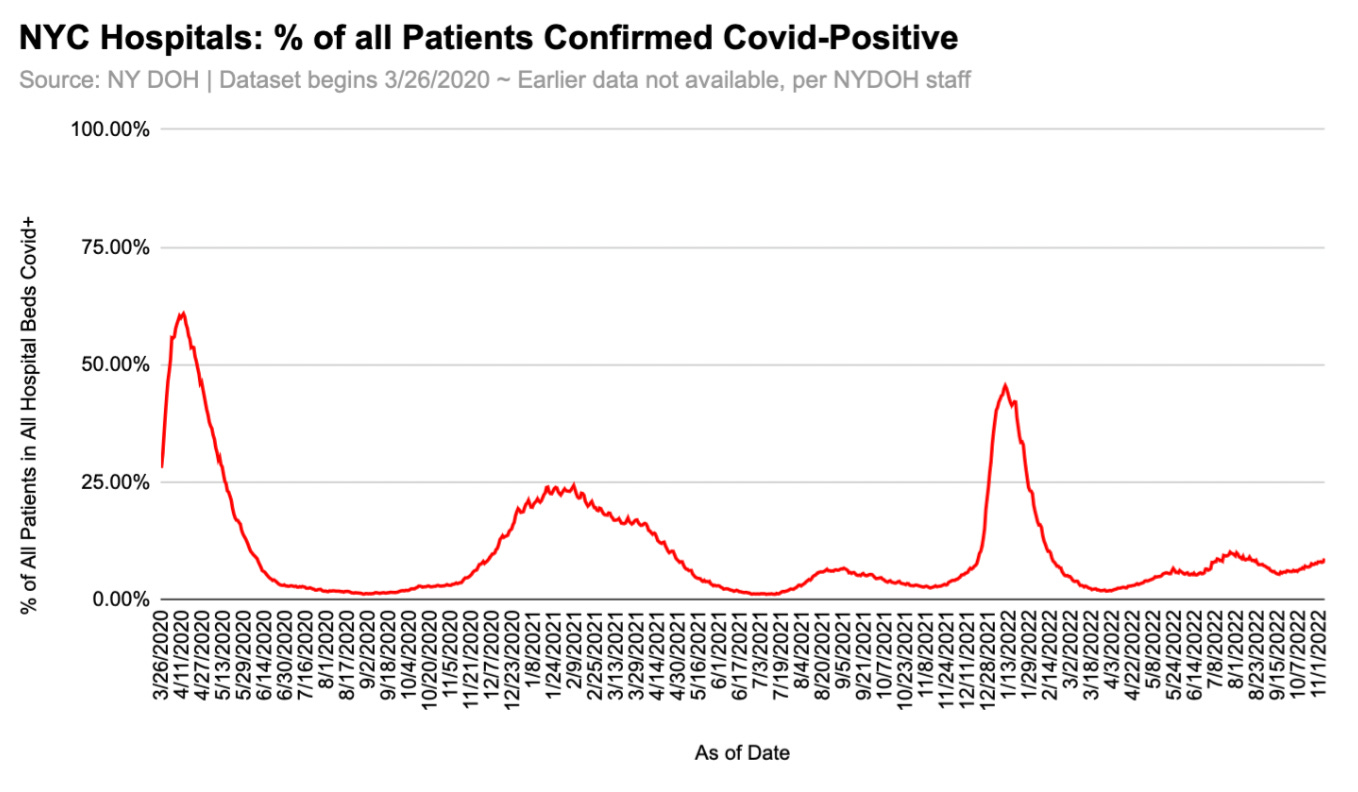
Patients Testing Positive for Covid-19 (SARS-CoV-2)
At peak, 60% of NYC Hospital inpatients in spring 2020 were confirmed covid-positive. Fascinating, isn’t it, that a few months after the *first* confirmed cases of SARS-CoV-2 in the U.S. were said to have been identified, there were 12,000 people in NYC hospitals who had a positive result on a highly-sensitive PCR test being run at presumably high cycle thresholds? Instead of seeing this percentage and thinking, “Maybe this virus has been circulating for awhile,” officials claimed it was evidence of sudden, uncontrolled spread that waited for lockdown orders to manifest itself in excess mortality, which is absurd on its face.
IMO, at minimum this ⬆️ is the result of myopically mass-testing everyone in the hospital for fragments of a virus — and providing financial incentives for positive results.
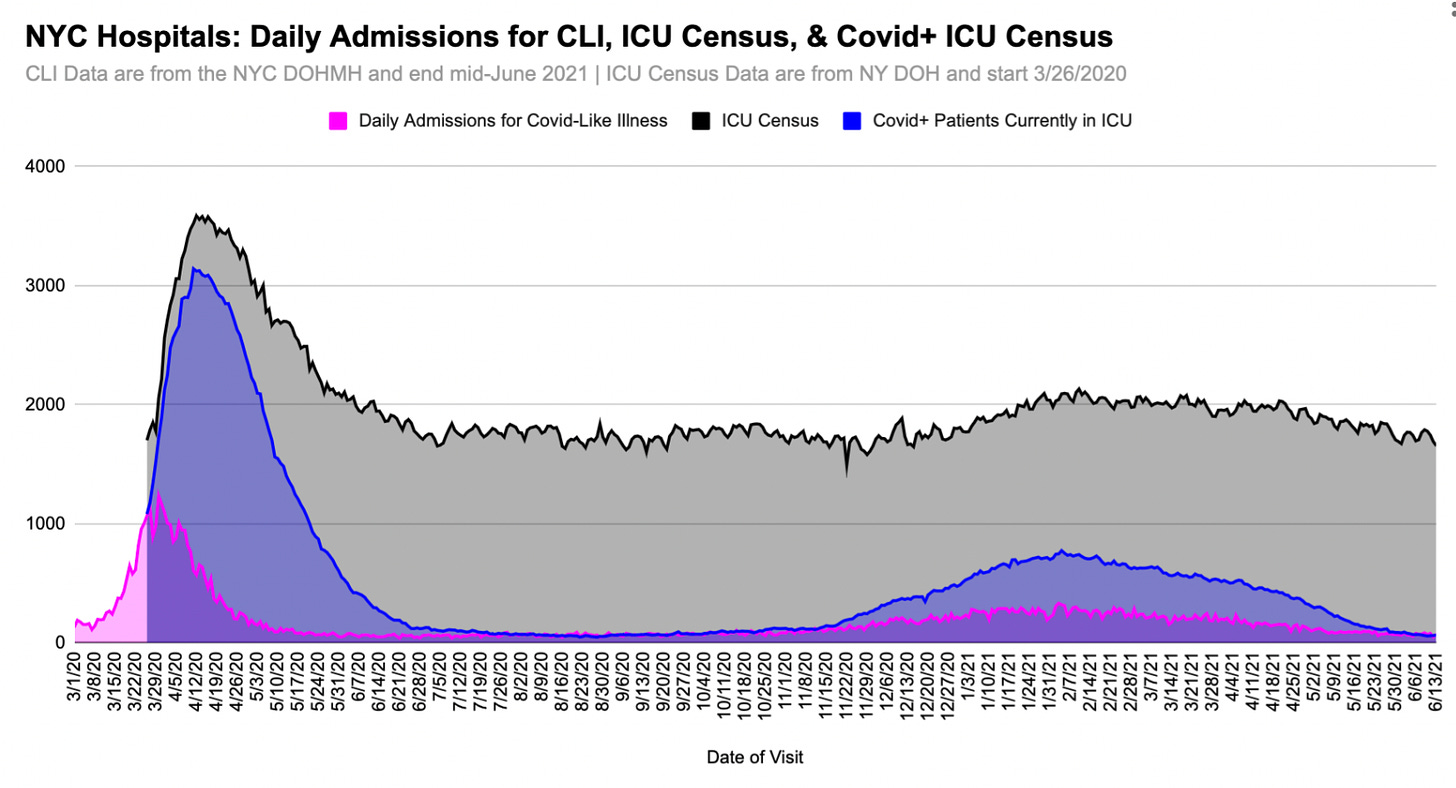
While we don’t know how many spring 2020 covid-positive patients were experiencing respiratory symptoms when they came to the hospital, data from the NYC Department of Health and Mental Hygiene on admissions for Covid-Like Illness6 is a decent proxy for the maximum number of actually-sick people.
Obviously, not all of those admissions - which topped out at 1,233 on March 30, 2020 - went to the ICU. Both back then and throughout the pandemic, most NYC covid-positive patients have been in acute-care beds. Until the January omicron wave subsided, 20%- 30% of all ICU patients were covid-positive.
The percent of acute-care and ICU patients testing positive has decreased appreciably since spring 2022. This decline could be attributable to changes in testing protocols, natural immunity, and other factors. (Positive flu tests are higher this season in NYC and elsewhere; I’d love to see the daily or weekly number of hospital-administered positive covid tests plus positive flu tests for the past few months.)
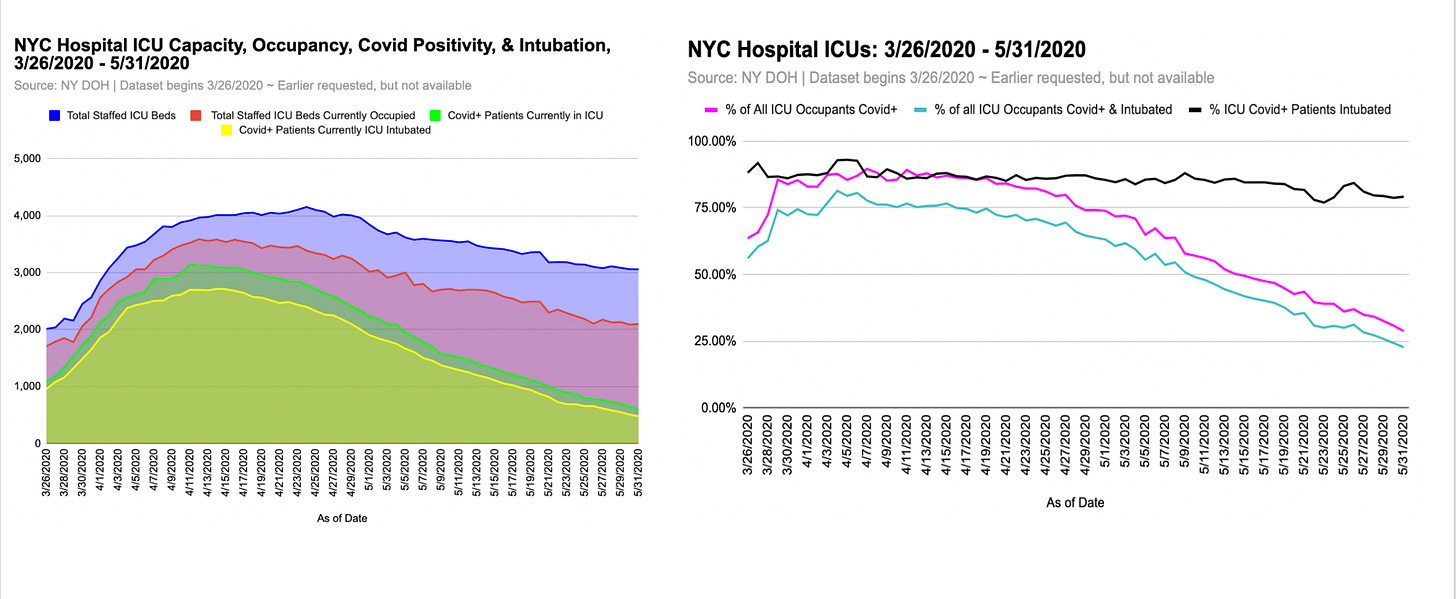
ICU Intubation
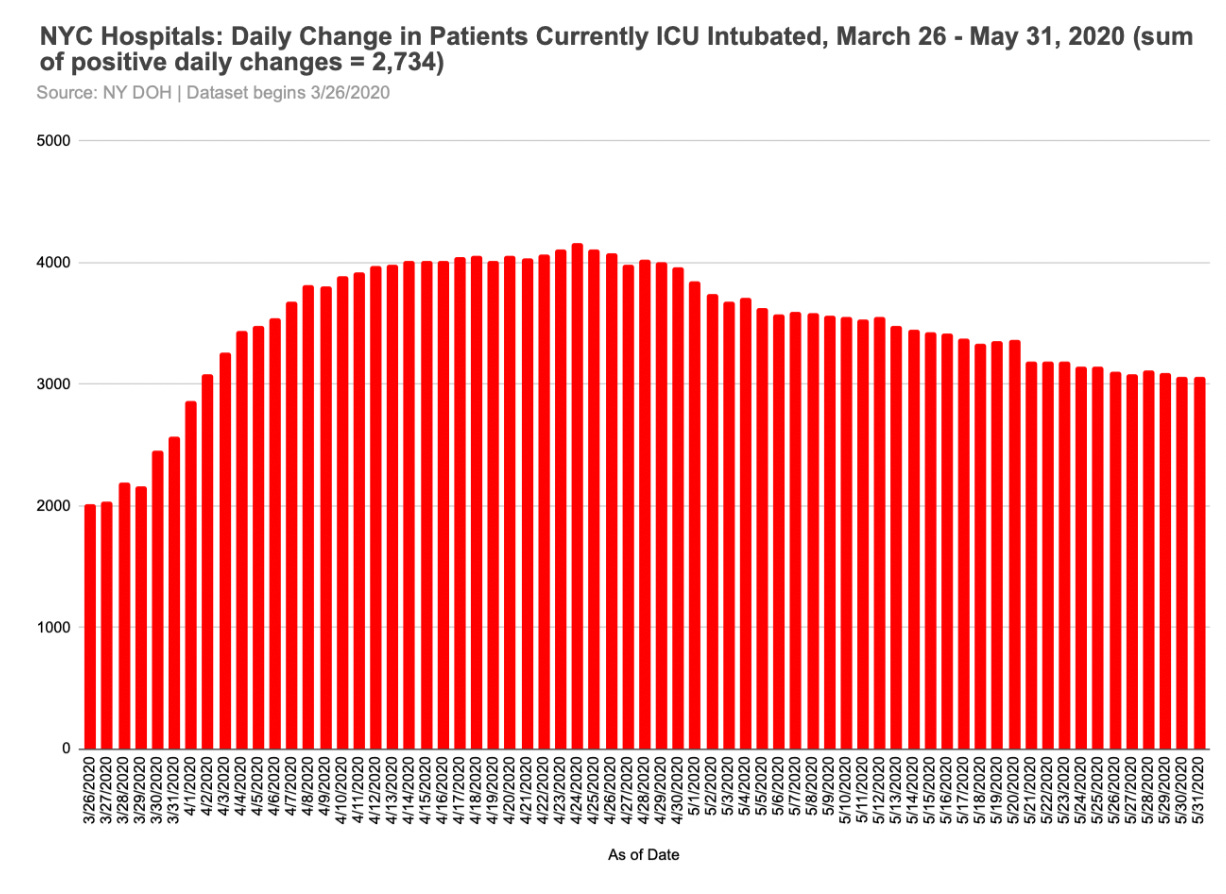
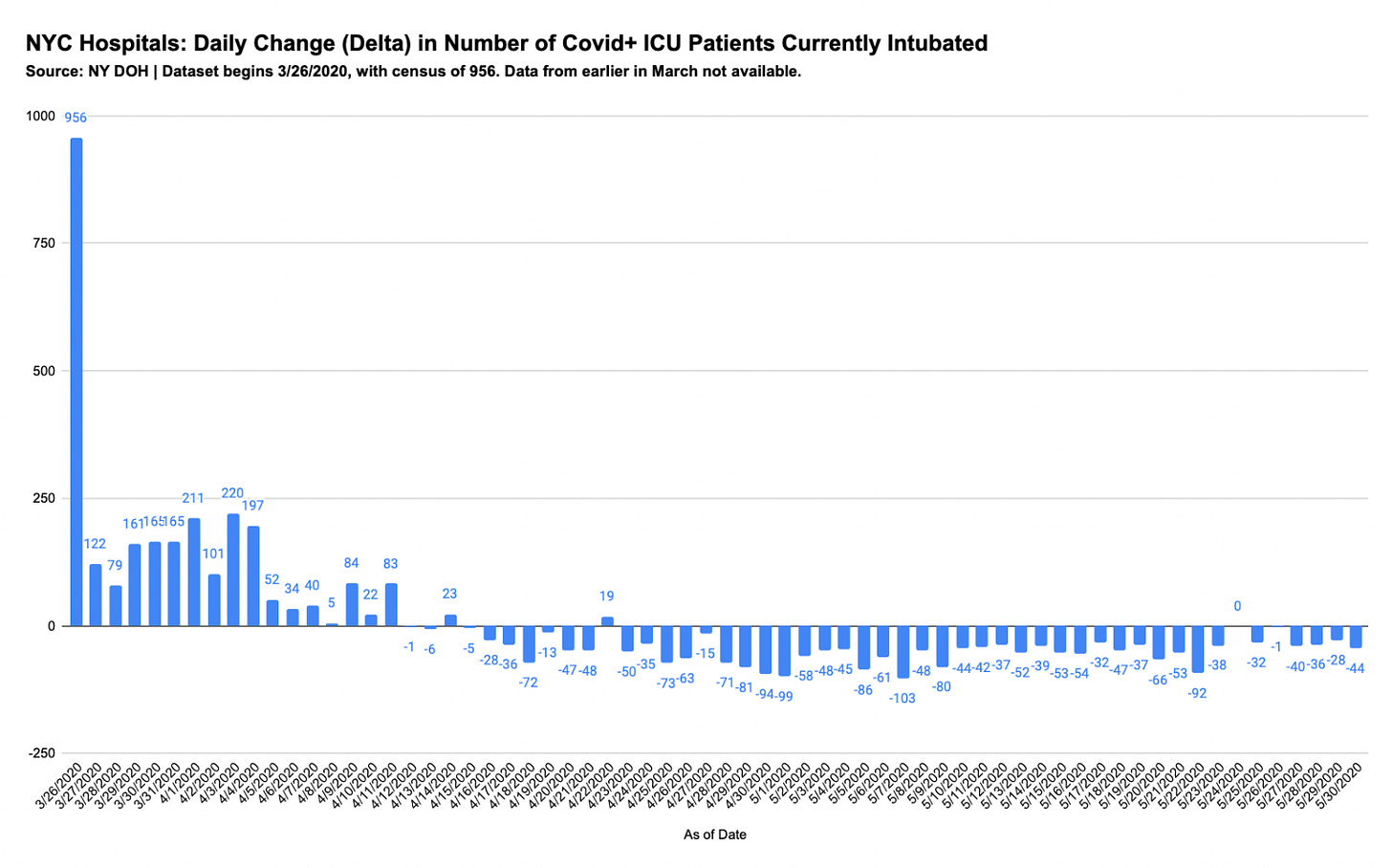
Most NYC hospital ICU patients in spring 2020 were covid-positive, and nearly all Covid-positive ICU Patients were intubated.
Unfortunately, the data don’t show us total number of hospitalized patients who were intubated at some point.
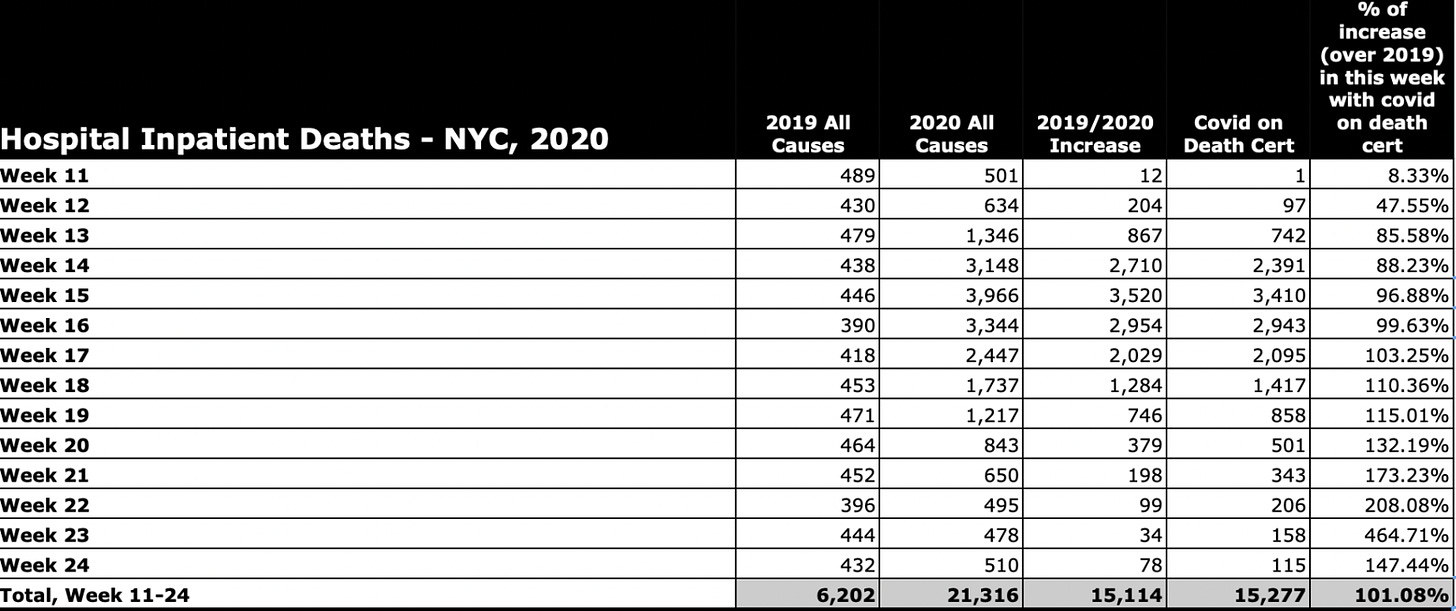
Still, the numbers bolster the claim that inappropriate use of ventilators with covid-positive patients, in accordance interim guidance from the World Health Organization, may have resulted in thousands of vent-assisted deaths - especially in New York City, which saw an astounding 244% increase in hospitals inpatient mortality in 14 weeks compared to the previous year.
Table source: CDC WONDER
As Michael Senger has noted, nearly all patients age 65+ in one early study of covid-positive patients in NYC-area hospitals placed on ventilators subsequently died.
It would be helpful for the New York Department of Health to require all hospitals in the state to report how many deaths of hospital patients with and without covid-19 on the death certificate were patients who were intubated at some point during their stay. The clamor over ventilators - and [mis]use thereof - in NYC and elsewhere may not only have needlessly killed thousands of people, but also painted a portrait of SARS-CoV-2 being much deadlier than it actually was…which in turn was used to justify and sustain harmful measures like keeping children out of school.
If ventilator use resulted in few deaths that wouldn’t have otherwise occurred, then it’s past time for New York (and other cities/states whose leaders followed its lead) to release the data prove it.
Data File
The raw data I used for this post is appended below. Readers are welcome to download, review, and comment with corrections, questions, and insights. My New York City inquiry is ongoing and benefits from credentialism-free feedback.
Note: Data downloaded November 7, 2020. Link to source included in Sheet 1. See source for data dictionary.
UPDATE: The original version of this article included an inaccurately-titled graph, “NYC Hospitals: % of All Bed Occupants that are Covid-Positive.” I replaced it with “NYC Hospitals: % of All Occupied Beds with Covid+ Occupants, Acute-Care v. ICU” and “NYC Hospitals: % of All Covid+ Patients by Bed Type”. Many thanks to reader MDskeptic for alerting me to the error.
This article is not focused on individual facilities. Specific hospitals will be the subject of future posts.
Thank you to Josh Stevenson for creating a file specific to NYC hospitals. We noticed there are missing days for recent months. It’s likely the data is continuously updated and is “back-filled” as data from various facilities is received.
It’s unclear if beds from temporary facilities such as the little-used, 2,500-bed Javits Center and USNS Comfort are included in the dataset
HERDS data for March 2020 through mid-July shows ~2,100 confirmed-covid nursing home resident deaths outside of facilities (i.e., in hospitals) in NYC. This number seems very low, given there were over 15,000 hospital inpatient deaths with covid on the death certificate in that timeframe, per CDC WONDER.
My attempts to procure it have been unsuccessful thus far. NY DOH told me via email on November 21, 2022, “There are no plans at this time to report data from earlier in 2020. It is likely the reporting system and the labs were not set up in time to report information from before that start date.”
Covid-Like Illness Admissions: “The number of hospital admissions for influenza-like illness, pneumonia, or include ICD-10-CM code (U07.1) for 2019 novel coronavirus. Influenza-like illness is defined as a mention of either: fever and cough, fever and sore throat, fever and shortness of breath or difficulty breathing, or influenza. Patients whose ICD-10-CM code was subsequently assigned with only an ICD-10-CM code for influenza are excluded. Pneumonia is defined as mention or diagnosis of pneumonia.”









The extreme death rates (relative to anywhere else in the world save Peru) coming out of Italy and NYC/NJ always perplexed me. I assumed it was a deadlier virus that just attenuated over time, thus a lower death rate by the time Texas got its wave. But appears, in NYC, NJ and Italy anyways, more likely to be iatrogenic. Death by treatment. Death by vent.
No surprise. My cousins wife is a nurse out of Portland and went to NYC for 12 weeks in 2020 to give relief to nurses there. She came back after 6 weeks. Every time they push the vaccine on me I ask “tell me again why your wife came back early from NYC”. That usually stops the conversation. There is also a great book out from a nurse in NY called undercover epicenter nurse who talks about her experiences at the elmhurst hospital.